Inpatient Medicine
General Comments: You will spend a significant portion of your clinical training caring for hospitalized patients. This environment presents different demands and opportunities then other areas of the healthcare system. Within the hospital, each branch of medicine has its own structure and approach. Several elements, however, are common to all:- Organization: Health care in teaching hospitals is very hierarchical. At the top of the pyramid is the attending physician, a staff doctor who has ultimate responsibility for the patient. Beneath them is the supervising resident, a physician in the advanced stages of their training. They supervise the interns, doctors in their first year out of medical school who are generally the worker bees of the service. Fourth year students (referred to as Sub or Acting Interns) may also be members of the team. This is their opportunity to work with an increased degree of autonomy in order to prepare them for their future role as doctors. Some teams have additional layers of residents or fellows (physicians participating in advanced post-residency training), depending on the complexity and volume of work to be done.
- Team Approach: Those at the higher levels function as managers while those in the trenches tend to focus on getting things done. However, this is also a system of graduated responsibility, allowing less experienced providers the chance to become increasingly involved in the decision making process over time.
- Role of the Student: The third year student occupies a variably placed position on the team. Clinical education is based on the concept that students learn through a process of observation and controlled participation in patient care. Their ability to function and contribute will depend on the scope of their general experience as well as specific knowledge in any one field. During the beginning of the year and/or early in a particular rotation, students will be less functional then towards the end. Furthermore, the very nature of some rotations (e.g. surgery) will pose obvious limits on the degree to which the student may actually participate. In addition, the student has a somewhat distinct position from the other team members in that their purpose is not merely to get work done. Nor, for obvious reasons, do they function with speed or efficiency, traits which frequently define the work of the other team members.
- Ask the head of your team (both resident and attending physician) for a precise description of your responsibilities. How many patients will you follow? Will you be writing admission H&Ps, daily notes, presenting at attending or work rounds, etc? Who will be reviewing your work?
- What are your expectations for the rotation? What are the most important things that you want to learn or experience? Even if these are no different then the other students (e.g. observe operations on a surgical service, practice putting in I.V.s, etc.), keep a mental list for yourself that you can refer to periodically. If you have unusual expectations that you feel can be reasonably met within the scope of the rotation, discuss them with your supervising physicians.
- With whom will you be working? One or several of the interns or with the resident directly? Make sure that you know how to contact them and that they know how to find you. It helps to confirm even the most obvious details as non-communication of what others feel is implicitly understood information can become the substrate for conflict.
- Offer feedback to your teachers. Let them know what works and what does not. Similarly, solicit input on your own performance. Don't leave this for the end of the rotation as by then you'll have lost the opportunity to incorporate suggestions and experiment with new approaches.
- Determine the weekly schedule of events. Are there student conferences or other commitments that will make you unavailable to the team? When and where are work rounds, radiology rounds, attending rounds, etc.? If you're on a surgical rotation, when will you be expected to be in the operating room?
- Identify when you are expected to be on call and what your exact responsibilities will be on those days. Will you be sleeping in the hospital? Who is responsible for informing you about new admissions? Should you see these patients with the rest of the team or interview them separately? If there are specific days that you need off, let your team members know at the start of the rotation.
- Realize that education is a two-way street. Students can and should contribute to the learning process. This is of particular value on fast paced rotations, when time constraints prevent other team members from being able to pursue this information on their own.
- Address conflicts or areas of dissatisfaction early in the rotation. Frequently, these are simply the result of miscommunication and can be easily remedied. More complex issues should be taken up either directly with the person(s) involved or, if you are uncomfortable with this approach, via the attending physician or course director. Don't let problems fester!
- Take each rotation seriously and try to learn as much as possible while you're there. A casual or cavalier attitude is rapidly transmitted to those with whom you work. Any lack of interest on your part will almost certainly lead to less enthusiasm and effort from your teachers. The resulting clinical experience is destined to be less fulfilling and interesting. Try to adopt the attitude that you are truly a practitioner in the field of medicine to which you've been assigned. The resulting experience will be more enjoyable, the teaching superior, and you may occasionally identify a previously undiscovered area of interest or aptitude.
Pre-Rounding: Work rounds occur each morning and are the time when the team sees each patient, discusses their course, and decides on the diagnostic and therapeutic plan of the day. In order to be maximally efficient, it falls to the students and interns to gather relevant clinical data. This process is referred to as pre-rounding and should incorporate the following:
- Review the flow chart that is kept for each patient. This sheet is a record of their vital signs as well as fluids taken in or excreted (referred to as Is and Os, for Ins and Outs) over a twenty-four hour period.
- Be aware of major events that have occurred over the past day. Were any studies performed? Were there major changes in clinical status? Of course, access to this information is predicated on your having been actively involved in the patient's care (i.e. you need to make it a priority to stay informed about the patient's clinical activity). If things are happening that you are not made aware of, mention this to the interns and residents so that they can help you become an active participant in the patient care process.
- Tracking down events that occurred overnight can be challenging. These can range from
evaluation of a fever to initiation of new medications. A few places to check:
- If your team was not on call, try to speak with the person who was responsible for caring for the patient overnight. Alternatively, it may be easier to check with your intern as they have, in all likelihood, obtained some sort of sign out from the covering person.
- Check the chart to see if any notes were written about specific overnight events (or by consulting physicians who may have stopped by late on the previous day). Also, take a look in the order section for things initiated over night. You may then be able to piece together what happened during your absence. If, for example, new antibiotics were given, then someone must have discovered a previously unrecognized infection.
- Speak with the nurse who was covering the patients overnight and/or the one who has taken over in the AM.
- Query the patient about any overnight events. You will need to perform a focused exam each morning, which is a prime opportunity to ask if anything has happened.
- Leave yourself plenty of time to pre-round. Early in the year, this can require up to 30 minutes per patient. You may need to arrive quite early, depending on your experience, as well as patient volume and complexity. However, providing yourself with a realistic time cushion will generate much less anxiety and allow you to be as complete and accurate as possible.
- Have instant access to each patient's relevant past history, medications and baseline labs.
- Be aware of in-house medications and daily lab results.
- Maintain a list of things that need to be done for each patient.
The following system allows you to keep all relevant information on 5x8 index cards. This method has several advantages:
- It's readily portable. The cards fit nicely into standard lab coat pockets and are available on most hospital floors.
- As opposed to clip-boards (which are frequently misplaced), these cards leave your hands free to perform tasks (e.g. physical examinations, compressions during CPR, etc.).
- It makes relevant data readily available and allows you to keep an organized list of things that need to be done.
- It's easily standardized and understandable by others.
- This system can be learned and used by students and then carried over and applied during later careers as house officers and attending physicians.
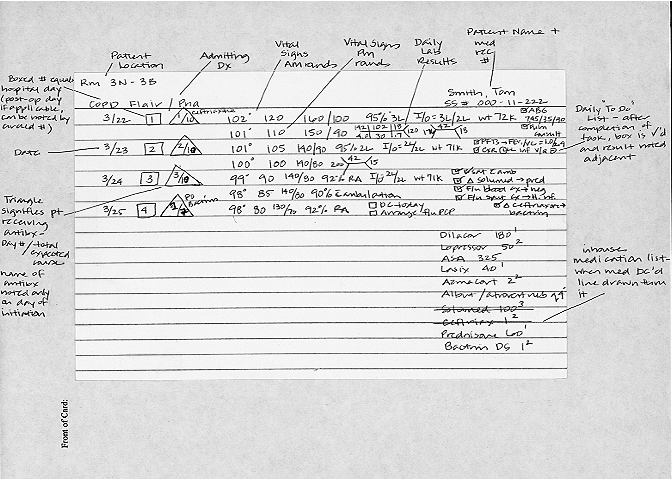
A few things to remember:
- Over time you will develop a short-hand that allows you to make best use of the card space available. You can also adjust the format any way you wish.
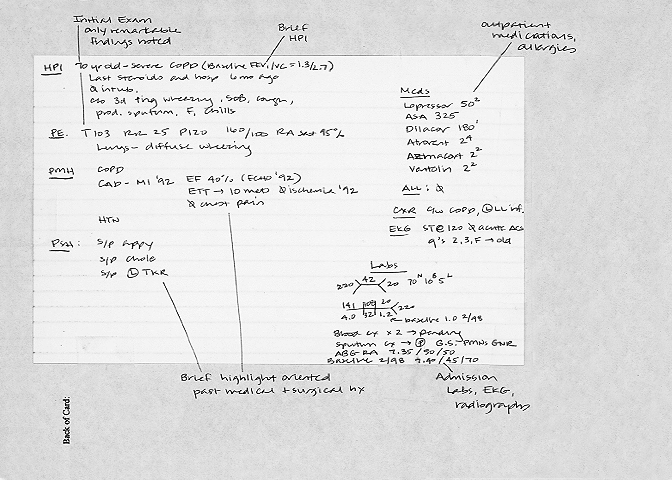
- The information included on the back (PMH, PSH, HPI, PE, etc.) is in very brief form. It should only include the critical highlights. More detailed points can be found in the chart.
- If a patient is hospitalized for a very long period of time, additional cards can be stapled on top of the original.
- The data presented should be factual. Old events that were described in earlier notes should not be repeated. The daily note is not meant to be a recapitulation of the H&P.
- The impression and plan generally reflects the thoughts of the entire team. That is, don't use the note as a format for expressing ideas that differ wildly from everyone else. If you don't understand, or even disagree with, the dominant view, talk to your team members and try to gain insight into their thought process. Independent reasoning is certainly encouraged. However, avoid using the note as a means of battling with (or inflaming) your colleagues. This is, unfortunately, a common problem for many "higher level" providers, leading to energy and time wasting "chart wars."
- Don't take hours (or more then 10 minutes, for that matter) to write a note. The length of the note will depend to a large extent on your experience, understanding of the case and the complexity of the patient's illness. However, there is generally WAY TOO MUCH attention paid to this process. Many, many other endeavors are of greater value, to both the patient and yourself. Remember, compared with all of the other aspects of patient care, the note is a minor end unto itself. After all, those most interested in the note are you and your team members. Thus, the exquisite detail found in many of these masterpieces is for the benefit of physicians who are already well aware of the patient and their course! In the event that some point is unclear, the reader can always find you to discuss the matter further.
- Make sure that you get feedback from team members about your written work.
- Certain services have very particular styles, emphasizing aspects that are important to the care that they provide. General Surgery teams, for example, tend to highlight fluid status, wound care, and IV access issues, areas that are critical to their patient population. Furthermore, these notes are very brief. The surgeon's time is spent elsewhere (e.g. the Operating Room) and by necessity they cannot spend exorbitant amounts of time charting. Realize that being succinct is not equivalent to being incomplete nor does it imply sub-optimal care. To my knowledge, no one has shown that the length of the note correlates with the quality of care delivered. In fact, it occasionally seems that more time and energy is put into notes then actual patient care!
Hospital Day # 3
- S: Patient feeling less short of breath, with decreased cough and sputum production.
- O: Maximum Temperature: 101.5 (yesterday 103)
- Pulse: 80-90
- BP: 110-120/70-80 RR: 20-24 Sat: 95% 2l O2 (yesterday 95% 4l O2)
- I/O: 2.5 L IV, 1 L PO/ UO 2L, BM x 1 Wt 140 lbs (no change from yesterday)
Day # 3 Ceftriaxone, 1g IV BIDPE: No jvd
Lungs: Crackles and dullness to percussion at R base with egophony; no change c/w yesterday
C/V: s1 s2 no s3 s4 m
Abd: soft, non-tender
Ext: no edema
Labs: Sputum and blood cx still negative; otherwise no new data
- Pneumonia: RLL pneumonia. Responding to IV Ceftriaxone, with decreasing
O2 requirement and fever curve. Also feeling better. No evidence of complications.
Plan:- IV abx x 1 addl day... then change to po Azithromax
- Hep. lock IV to assess if PO intake adequate
- Check sat off O2... d/c if under 92%
- Encourage ambulation
- consider discharge in approximately 2 days if continues to improve.
That's a pretty simple note. However, it clearly serves its purpose. More complicated patients with additional issues would require an assessment and plan that dealt with each problem specifically. Notice that I've chosen to highlight objective data so that improvement is clearly demonstrated (e.g. decreased O2 requirement, declining temperature curve) and number ranges are mentioned when discrete points in time might not be representative (e.g. for heart rate and blood pressure). This is based on common sense and is done at the discretion of the writer. In addition, I chose to mention the antibiotic given and duration of therapy to date. In this case, it's an important issue and deserves mention. The patient may be receiving other medications, perhaps for the treatment of several chronic conditions (e.g. hypertension, glaucoma, etc.). As these elements were undoubtedly mentioned elsewhere and are not changing, I've omitted them from the SOAP note. If, however, there was ongoing medication adjustment, as might be the case if Insulin were being used to treat diabetes or extra doses of Lasix provided for heart failure, I would have made special mention of these meds as well.
Presenting During Work Rounds: The formal, complete oral presentation is discussed elsewhere. Work rounds are, of course, for work. Regardless of the service, time constraints demand that presentations be succinct yet thorough. An average presentation should take no more then a few minutes. The following is a sample presentation for a patient on the General Surgery service:
"Mr. Smith is post operative day #2 from his appendenctomy, day #3 of 7 of Ampicillin, Gentamycin and Flagyl.A few things are worth highlighting:Events over the past 24 hours include:
Patient appeared comfortable, without specific complaints
- CXR performed as part of a fever evaluation; no pulmonary pathology identified
- Passing of flatus.
- Decreased abdominal pain.
Vital Signs:Lungs: Clear
- T Max 102.5 yesterday, 100 over past 8 hours
- Heart Rate 80s to 90s, Blood Pressure 120s-140s over 70s
- Respiratory Rate in low 20s, Sat'ing at 95% on Room Air
- Weight 150 pounds, down 1 pound from yesterday; still up 5 pounds from pre-op
- Is and Os: 2L IV NS at rate of 100/hour. Additional 500 ccs IVF from antibiotics. Still NPO. Urine Output total 2 L, approximately 50 cc/h.
Heart: regular rate and rhythm without murmurs
Abdomen: hypoactive bowel sounds now present; slightly distended; wound without erythema or discharge; minimal pain at incision siteLabs: This morning's Chem 7 and CBC pending; Yetsterday BUN and Creat 11 and .8, which are consistent with baseline; White count 16, down from 20 the previous day. Intra-operative cultures still negative; blood and urine cultures from day of admission and yesterday negative.
(Team may or may not take this opportunity to enter the patient's room for group interview and exam)
Assessment and Plan:
- G.I. (gastrointestinal): Patient S/P appendectomy. Had prolonged ileus associated with significant peri-appendiceal inflammation. Now with apparent recovery of gut function as evidenced by flatus, bowel sounds.
Plan:
- Advance to sips of clear liquids this A.M... If tolerated, will allow full clears this afternoon and then hep. lock IV as appears to be euvolemic.
- Encourage ambulation around floor
- I.D. (Infectious Disease): Recurrent post operative fever, presumably secondary to residual peri-appendiceal infection. Fever curve now trending down, white count decreasing, and improving clinically. Cultures from all other sources negative. Exam does not suggest infection elsewhere.
Plan:
- Continue current antibiotics for additional 24 hours. If remains well, change to oral ciprofloxin and flagyl to complete 7 day course.
- Follow up on cultures.
- Ambulation and incentive spirometry may help if atelectasis contributing.
- T/L/D (Tubes, Lines, and Drains): Patient has adequate IV access. Foley catheter still in palce.
Plan:
- D/C Foley
- Dispo (Disposition):
Plan:
- Expect patient may be ready for discharge in 2 days
- Every service has a different style. Some may see every patient as a group and discuss the assessment and plan after the exam. Others prefer to hear the entire presentation (including the A and P) prior to seeing the patient, with appropriate adjustments made after the visit. The only way to learn the particulars is to ask.
- Oral presentations do not precisely follow the SOAP format. In the above example I've opted to include an "events" section along with the Subjective comments. Patients presented for the first time will generally be done in a more inclusive fashion, covering enough background information so that the course to date as well as the assessment and plan are understandable to all team members.
- Accurate presentations require that the presenter be intimately aware of all the details related to a patient's course. Pre-rounding and record keeping (see above) are thus vital. You'll also find it necessary to read critical data from your portable record keeping system.
- You may find it helpful, particularly early in your careers, to take a few minutes before rounds to practice your presentations.
- The number of sub-categories mentioned in the assessment and plan will vary with the complexity of the patient's illness. Patients with many issues will require detailed discussions. The major categories include: Neurological, Cardiac, Pulmonary, gatrointestinal, Renal, Hematologic, Infectious Disease, Endocrine/Metabolic, Access (i.e. tubes, lines, and drains), and Disposition. If there are no issues related to a particular area, it is not mentioned in the discussion. At times, there will be clinical problems that bridge several areas. For example, pneumonia is both a Pulmonary and an ID issue. In such settings, the presenter uses their judgment and discusses the problem under a single heading in order to avoid redundancy. In very complex cases, these major headings can be exploded into sub- categories so that important issues are not missed. For example, a patient may have CHF, Hypertension and Atrial Fibrillation. These are all Cardiac issues, which may or may not be related. As each requires specific therapy, listing them separately allows for maximum clarity.
- It will take some time before you become comfortable presenting as this process requires rather advanced organizational skills. In addition, you are likely to feel quite exposed during this process. Try not to be intimidated or discouraged. Ask for feedback frequently.